A Thrombus, or blood clot, is the final product of the blood coagulation step in haemostasis. There are two components to a thrombus: aggregated platelets that form a platelet plug, and a mesh of cross-linked fibrin protein. A thrombus is a healthy response to injury intended to prevent bleeding, but can be harmful in thrombosis, when clots obstruct blood flow through healthy blood vessels.
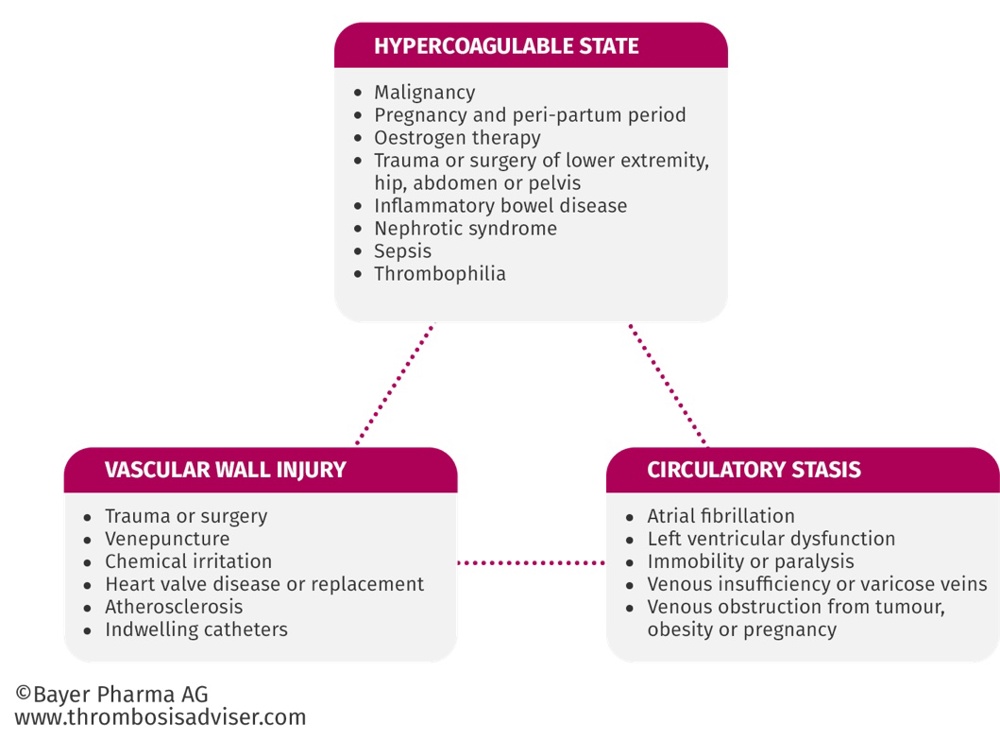
Virchow’s triad describes the pathogenesis of thrombus formation:
- Endothelial injury (injury to the endothelial cells that line enclosed spaces of the body, such as the inside of blood vessels (e.g. trauma, atheroma)
- Abnormal blood flow (loss of laminar flow resulting from stasis in veins or turbulence in arteries (e.g. valvulitis, aneurysm)
- Hypercoagulability (e.g. leukaemia, Factor V mutation (Leiden)
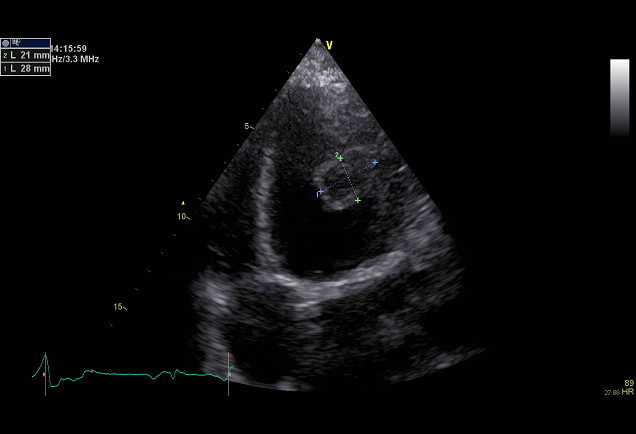
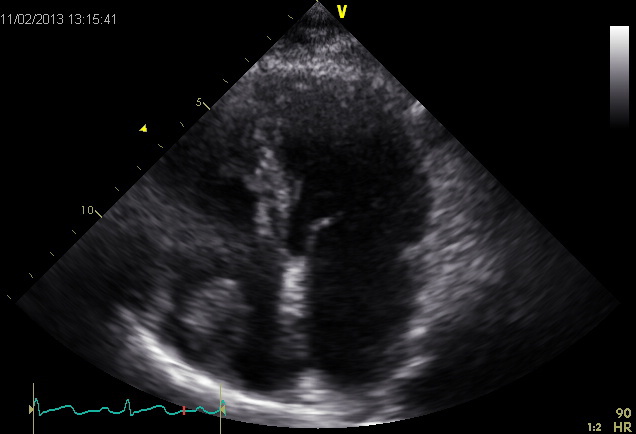
According to Virchow’s triad, intracardiac thrombus formation can be enhanced in the setting of post-myocardial infarction remodelling, in which mural thrombi can form in an aneurysmatic LV apex or in apposition to an akinetic myocardial wall. In the setting of atrial fibrillation, atrial contractility is compromised and thrombus formation can be enhanced inside the left atrial appendage. Presence of intracardiac thrombi is associated with increased risk of pulmonary or systemic embolism. Approximately 20% of ischemic strokes are thought of to be of cardiac origin. Hence, presence of intracardiac thrombi represents an indication for anticoagulation therapy.