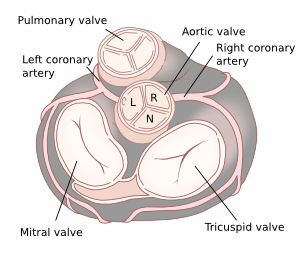
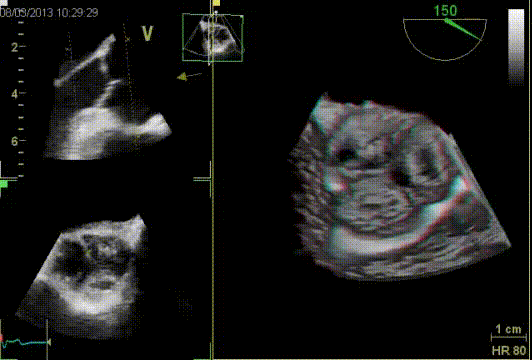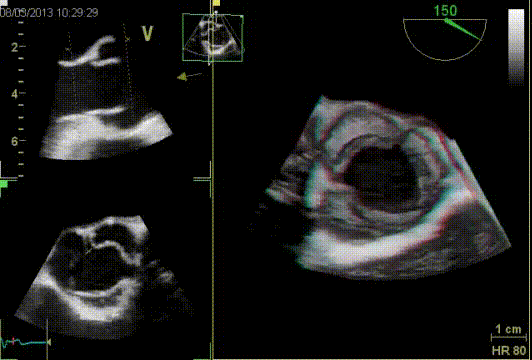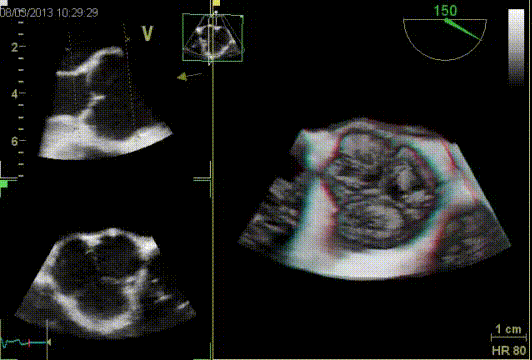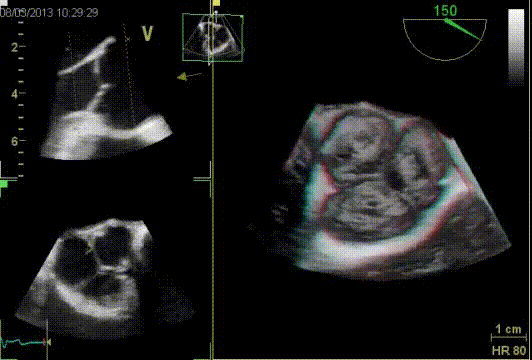
Quantification of aortic valve regurgitation
| AR severity classes(a) |
Mild |
Moderate |
Moderate |
Severe |
| |
grade 1 or 1+ |
Grade 2 or 2+ |
Grade 3 or 3+ |
Grade 4 or 4+ |
| Qualitative parameters |
| Aortic valve morphology |
Normal/abnormal |
Normal/abnormal |
Abnormal/prolaps/moderate coaptation defect |
Abnormal/flail/lage coaptation defect |
| Colour flow AR jet width(b) |
Small in central jet |
Intermediate |
Large in central jet, variable in eccentric jets |
Large in central jet, variable in eccentric jets |
| Colour flow convergence |
None or very small |
Intermediate |
Intermediate |
Large |
| CW signal of AR jet |
Incomplete/faint |
Dense |
Dense |
Dense |
| Diastolic flow reversal in descending aorta |
Brief, proto-diastolic flow reversal |
Intermediate |
Holodiastolic flow reversal |
Holodiastolic flow reversal |
| |
|
|
end-diastolic velocity 10 to <20 cm/s |
end-diastolic velocity ≥20 cm/s |
| Diastolic flow reversal in abdominal aorta |
Absent |
Absent |
Present |
Present |
| Semi-quantitative parameters |
| Vena contracta (mm) |
<3 |
3-6 |
3-6 |
>6 |
| Jet width/LVOT diameter (%) |
<25 |
25-45 |
46-64 |
>65 |
| Jet CSA / LVOT CSA (%) |
<5 |
5-20 |
21-59 |
≥60 |
| Pressure half time (m/s)(c,d) |
>500 |
500-200 |
500-200 |
<200 |
| Quantitative parameters |
| EROA (mm²) |
<10 |
10-19 |
20-29 |
≥30 |
| R Vol (mL) |
<30 |
30-44 |
45-59 |
≥60 |
| RF (%) |
<30 |
30-39 |
40-49 |
≥50 |
| Structural parameters |
| LV size(e) |
Usually normal |
Normal or dilated |
usually dilated |
usually dilated |
AR, aortic regurgitation; CSA, cross-sectionnal area; CW, continuous wave; LA, left atrium; EROA, effective regurgitant orifice area; LV, left ventricle; RF, regurgitant fraction; R Vol, regurgitant volume; VC, vena contracta.
(a)Grading of severity of AR classifies regurgitation as mild, moderate or severe, and sub-classifies the moderate regurgitation group into two subclasses: ‘mild-to-moderate’ (EROA of 10–19 mm or a R Vol of 20–44 mL) and ‘moderate-to-severe’(EROA of 20–29mm or a R Vol of 45–59mL).
(b)At a Nyquist limit of 50–60 cm/s.
(c)These parameters are influenced by LV and aortic compliance. Hence, low transvalvular end-diastolic aorta to LV pressure gradient due to concomitant moderate/severe LV diastolic dysfunction may lead to false positive results. The high dependency of aortic flow reversal on aortic compliance considerably limits the utility of this parameter in the elderly population. These parameters are also influenced by chronotropy.
(d)Pressure half-time is shortened with increasing LV diastolic pressure, vasodilator therapy, and in patients with a dilated compliant aorta or lengthened in chronic AR.
(e)Unless for other reasons, the LV size is usually normal in patients with mild AR. In acute severe AR, the LV size is often normal. Accepted cut-off values for non-significant LV enlargement: LV end-diastolic volume <82 mL/m2, LV end-systolic diameter <40 mm2, LV end-systolic volume <30 mL/m2.